When you have diabetes, high blood sugar can take a toll on your entire body — including your teeth and gums. You are 3 to 4 times more likely to develop gum disease, with a higher rate of severe bone loss and gum infections.
When you have diabetes, high blood sugar can take a toll on your entire body — including your teeth and gums. You are 3 to 4 times more likely to develop gum disease, with a higher rate of severe bone loss and gum infections.
Diabetes and Your Mouth
With Diabetes you are at higher risk for-
- Dry mouth: When your salivary glands don't produce sufficient saliva to keep your mouth moist, your mouth can become inflamed and sore. It can make chewing, tasting, and swallowing more difficult, as well as cause difficulty in eating, making it more difficult to control blood sugar.
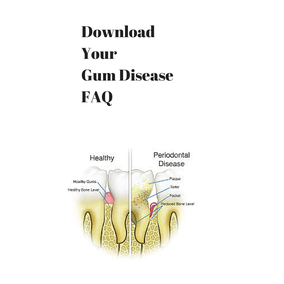
- Gum inflammation: Diabetes reduces your ability to fight bacteria. If you don't remove plaque with regular brushing and flossing, it'll harden under your gum line into a substance called tartar (calculus). The longer plaque and tartar remain on your teeth, the more they irritate the gingiva — the part of your gum around the base of your teeth. In time, your gums become swollen and bleed easily. This is gingivitis.
- Advanced gum disease (periodontitis): Left untreated, gingivitis can lead to a more serious infection called periodontitis, which destroys the soft tissue and bone that support your teeth. Eventually, periodontitis causes your gums to pull away from your teeth and your teeth to loosen and even fall out. Periodontitis tends to be more severe among people who have diabetes because it lowers their ability to resist infection and slows down healing. An infection such as periodontitis may also cause your blood sugar level to rise, which makes your diabetes more difficult to control. Preventing and treating periodontitis can help improve blood sugar control.
- Oral surgery complications: If you need oral surgery, diabetes— particularly if poorly controlled—can complicate oral surgery. Diabetes retards healing and increases risk of infection. Your blood sugar levels also may be harder to control after oral surgery. Your dentist should work closely with your doctor to minimize possible complications.
- Thrush: Candida albicans is a fungus that normally lives inside the mouth without causing problems. But when you have diabetes, deficient saliva in your mouth and extra sugar in your saliva allow the fungus to cause thrush, which appears as sore white or red areas in your mouth.
- Tooth decay: Bacteria in the mouth produces acids from sugars in the diet. Tooth decay happens when these acids remove minerals from the hard outer surface (enamel) of the tooth. The area becomes weaker and a hole may develop, sometimes causing toothache. The higher your blood sugar level, the greater the supply of sugars and starches — and the more acid wearing away at your teeth.
How to ensure good dental hygiene as a diabetic
Proper brushing takes at least two minutes — that's right, 120 seconds! Most adults do not come close to brushing that long. A soft-bristled brush is best for removing plaque and debris from your teeth. Small-headed brushes are also preferable, since they can better reach all areas of the mouth.
It is important that you use a toothpaste that's right for you. Today there is a wide variety of toothpaste designed for many conditions, including cavities, gingivitis, tartar, stained teeth and sensitivity. Ask your dentist or dental hygienist which toothpaste is right for you.
Replace your toothbrush when it begins to show wear, or every three months, whichever comes first. It is also very important to change toothbrushes after you've had a cold, since the bristles can collect germs that can lead to reinfection.
Visit your dentist every six months
Making sure that you visit your dentist every six months ensures that any infection will be treated as early as possible. Minor dental problems can quickly escalate, and a routine visit to the dentist will pick up on these.
Keep your dentist up-to-date on your diabetic condition and your doctor up-to-date on your oral condition.
If your diabetic condition is well controlled, periodontal treatment would be the same for you as for a patient without diabetes.


.png?width=320&name=Request%20(1).png)